Navigating the Storm
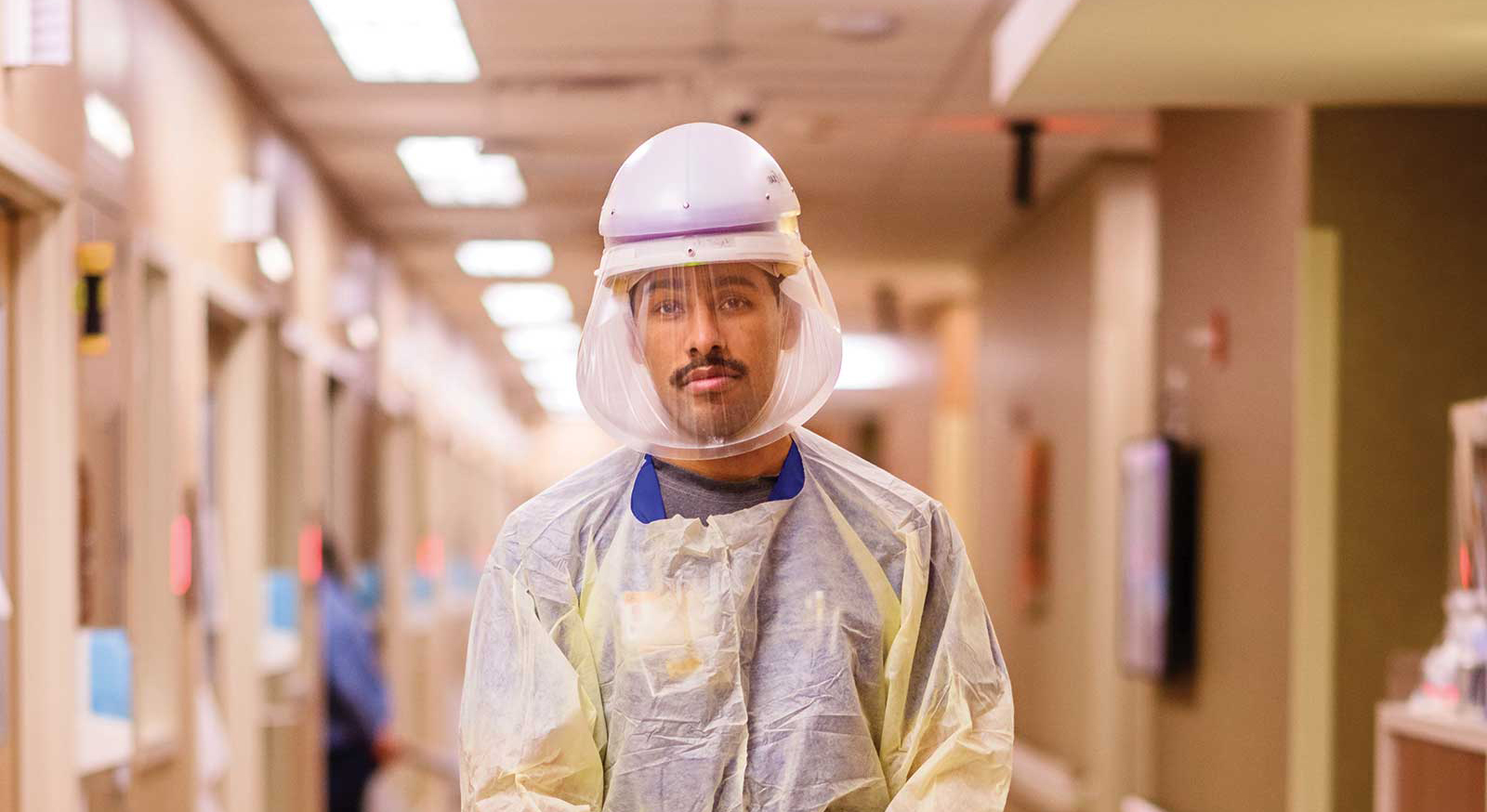
Columbia nurses rise to the challenges of a global pandemic.
Nurses are used to a fast-paced, constantly changing, and stressful environment, but COVID-19 has challenged health care workers in a whole new way. Columbia’s nurses have risen to that challenge by providing competent and compassionate care while finding the encouragement and hope they need to return to the hospital shift after shift.
Kaitlyn Kral

She’s still working the same number of hours each week, but for Kaitlyn Kral, a registered nurse in University Hospital’s progressive care unit, those 36 hours feel much longer and harder than they did before COVID-19 hit Columbia.
“I’m absolutely exhausted,” Kaitlyn says. “I think I can speak for a lot of my co-workers. We are tired. We are exhausted. I work the night shift, and it takes me two days to recover from a shift.”
Kaitlyn never dreamt she would be a first-year nurse in the middle of a pandemic, but that’s exactly what’s happened. She began her nursing career at University Hospital in July 2019 and says she enjoyed her job in the progressive care unit, which served as a middle ground between the ICU and the step-down unit. She spent her nights caring for a variety of patients — those admitted from the ER, those recovering from surgery, and those with infections like pneumonia.
Less than a year later, her unit transformed into the COVID-19 unit, and nursing as she knew it completely transformed.
“It has changed in so many ways,” Kaitlyn says. “With the PPE we have to wear now, it takes us a lot longer to get into patient rooms with the gloves, gowns, and goggles. We are clustering care, so we have to be conscious of everything we need to do in a patient’s room. We try to conserve PPE, so we try to think of everything we need and bring it all into the room at once.”
Though nursing is always a stressful profession, refuges from work have become an even more important part of nurses’ lives this year — at the same time, doing certain things to unwind has become difficult or impossible due to the pandemic. Kaitlyn says binge-watching television and doing puzzles has become her way of decompressing in a time when she can’t hang out with friends. She says being part of a close, strong team at work means that she has a good support network, and talking about what happened the night before helps her process what she’s experienced and prepare for her next shift.
“I will give myself a limit for how long I can talk about something with my co-workers,” she says. “After a shift, we will vent, get it all out, talk about the hard things we’ve seen or had to deal with that shift, and then try to forget it. Sometimes it works, but not always. There are some things that you see at work that you don’t ever forget.”
Xavier Scott

Xavier Scott also works nights on University Hospital’s progressive care unit. Despite his one and a half years of experience on the floor prior to COVID-19, he says that when the unit transformed into the hospital’s COVID-19 unit, it was a new experience for everyone.
“It was an anxious feeling going into work because you didn’t know what it would be like,” Xavier says. “I had worked with easily spreadable diseases before as a nurse, but it was a new experience trying to care for our patients while keeping staff and the community safe.”
One of the hardest parts of nursing in the age of COVID-19 is that patients are separated from family members, who often serve as a source of comfort and as advocates. Being separated from their families adds to patient anxiety, so Xavier says he spends a lot of time calming them down as much as possible.
“We are the only people they see in person while they’re in the hospital, and it’s hard not having family members there to help them,” he says. “Part of my job at night is to try to let people sleep, but I also try to talk to them and give them company. It can get lonely when you’re stuck in a room all day with not much to do.”
Outside of work, Xavier tries to avoid news about the virus. He’s found an escape in reading and in researching and building a new computer for gaming. His wife, also a registered nurse, is another big source of comfort to him, as she understands the nuances of patient care.
“I’ve witnessed more patients dying in the past few months than I had in my first year and a half as a nurse,” he says. “I try to talk about my day with my wife and other nurses, and faith is a big part of my life. I also realize that my job is to help people, and when there’s not much else that can be done or things that families don’t want to do anymore, I can help them pass in a way that allows their families to say their goodbyes and let [patients] keep their dignity and be comfortable.”
Rachel Jennings

Rachel Jennings is the medical specialties supervisor at Boone Hospital Center. While she’s always stepped in to care for patients around the hospital as needed, she has found herself involved with direct patient care much more frequently since the pandemic hit Columbia. Despite her 10 years of experience caring for patients as a nurse, she says COVID-19 has brought with it a whole new learning curve.
“We’re always acutely watching patients, but these patients can change quicker than I’ve ever seen,” Rachel says. “They can be fine, breathing room air, and within hours, they need to go to the ICU and be intubated. It is different in every patient, and you never know what will happen. You can’t look at an 80-year-old or a 30-year-old and say who is going to make it. That takes its toll.”
As nurses focuses their complete attention on patients, Rachel says communicating with anxious family members has become more important — and challenging — than ever. She and her colleagues have found the delicate balance between sharing updates with families and being available for patients by designating hours of their time to make phone calls.
“You have phone calls coming in all day long from family members, and you can’t leave the room to get the phone,” Rachel says. “You understand what they’re wanting to know and why they’re calling, but balancing that has been stressful.”
Despite long, hectic days at the hospital, Rachel says she and her colleagues have become an even closer team, relying on each other for a laugh or support throughout the day. Outside of work, they’ve created Facebook groups to help one another find ways to be healthier.
“One of the hardest things, now that we’ve been doing it for so many months, is feeling isolated,” Rachel says. “We were a floor that constantly had therapists, volunteers, and doctors. We hardly see anyone anymore. The social aspect is gone for patients and for us.”
As she continues to navigate the challenges of nursing during a pandemic, Rachel says she has been touched by an outpouring of appreciation from patients, their families, and the community, and she is prouder than ever to be a nurse.
“I’m proud of my profession and the team I work with,” she says. “None of us expected this, but we have all dug in and given it our all.”
Stephanie Bernard

The primary care coordinator at Harry S. Truman Memorial Veterans’ Hospital, Stephanie Bernard got a sneak peek into Columbia’s future when she deployed to Maryland in April and Mississippi in September as part of a VA effort to provide relief for overworked nurses.
“It was a big eye-opener,” Stephanie says. “When I went, we hadn’t had a surge here in Columbia, but in Maryland, they were completely shut down and at the height of their surge. I got to bring back a lot of knowledge about what they were seeing symptom-wise and what they were doing with PPE. It was really helpful.”
Leaving town for her deployments meant that Stephanie’s husband had to take on more responsibilities at home, including taking their 7-year-old daughter to school. Friends, family, and co-workers stepped up to support her family — support that was integral to her ability to deploy. Although the pace was fast and the environment and care protocol was constantly evolving, Stephanie says the experience of a deployment, and being able to bring relief to an overworked facility, was personally and professionally fulfilling.
“It was very rewarding,” she says. “You get there, and the staff is so happy to have help, it gives them new hope that we are going to beat this and that things will be okay.”
Although she’s been a nurse for 11 years, Stephanie says nursing during COVID-19 looks different than anything she’s seen. Walking into a patient room used to involve simple hand-washing and putting on a pair of gloves rather than the methodical assessment of the necessary PPE.
“The care is a lot different than what I did 10 years ago on the floor,” she says. “The patients are a lot sicker, there are a lot more unknowns about symptoms, and it presents differently than any disease we’ve known.”
As the vaccine provides a recharge and the glimmers of hope that she and other nurses need to keep pushing through the pandemic, Stephanie says she has found comfort in support from nursing school friends and other nurses, including a nurse she met while deployed in Maryland.
“We check on each other to make sure everyone’s health, [including] mental health, is stable,” she says. “Everything was different last year, but now there is new hope for 2021.”